Whether you’re hiring a full-time employee (FTE) or virtual assistant (VA), certain core aspects of compliance and security remain the same. After all, regulations like the Health Insurance Portability and Accountability Act (HIPAA) apply to all healthcare personnel, irrespective of their geographic location or employment status. Similarly, data security principles, such as encryption and secure access controls, are universally applicable.
However, there are additional complexities when dealing with VAs, particularly those overseas. For instance, cross-border data transfers could potentially expose patient records to different jurisdictions and varying degrees of data protection standards. Time zone differences might also affect how promptly VAs can respond to security incidents or compliance inquiries.
Eye care practice owners must consider nuances such as their VAs’ roles and impact on data management, ensuring continuity of health care, and more. For a broader look at meeting regulatory requirements, see our guide on strategies to uphold legal and regulatory compliance in optometry. Our practical insights below will help you get a sense of how your clinic can remain compliant and secure when using VAs. It’s a good primer before a discussion with your legal and IT teams/partners.
Table of Contents
- How Does the Role of Virtual Assistants Impact Data?
- How Do You Secure Communications and Data Management?
- How Should You Manage Data Backups and Recovery?
- How Do You Navigate Cultural and Language Differences?
- How Do You Ensure Continuity of Care with Virtual Assistants?
- What Ethical and Contractual Considerations Apply?
- Walking the Walk of Compliance and Data Security
How Does the Role of Virtual Assistants Impact Data?
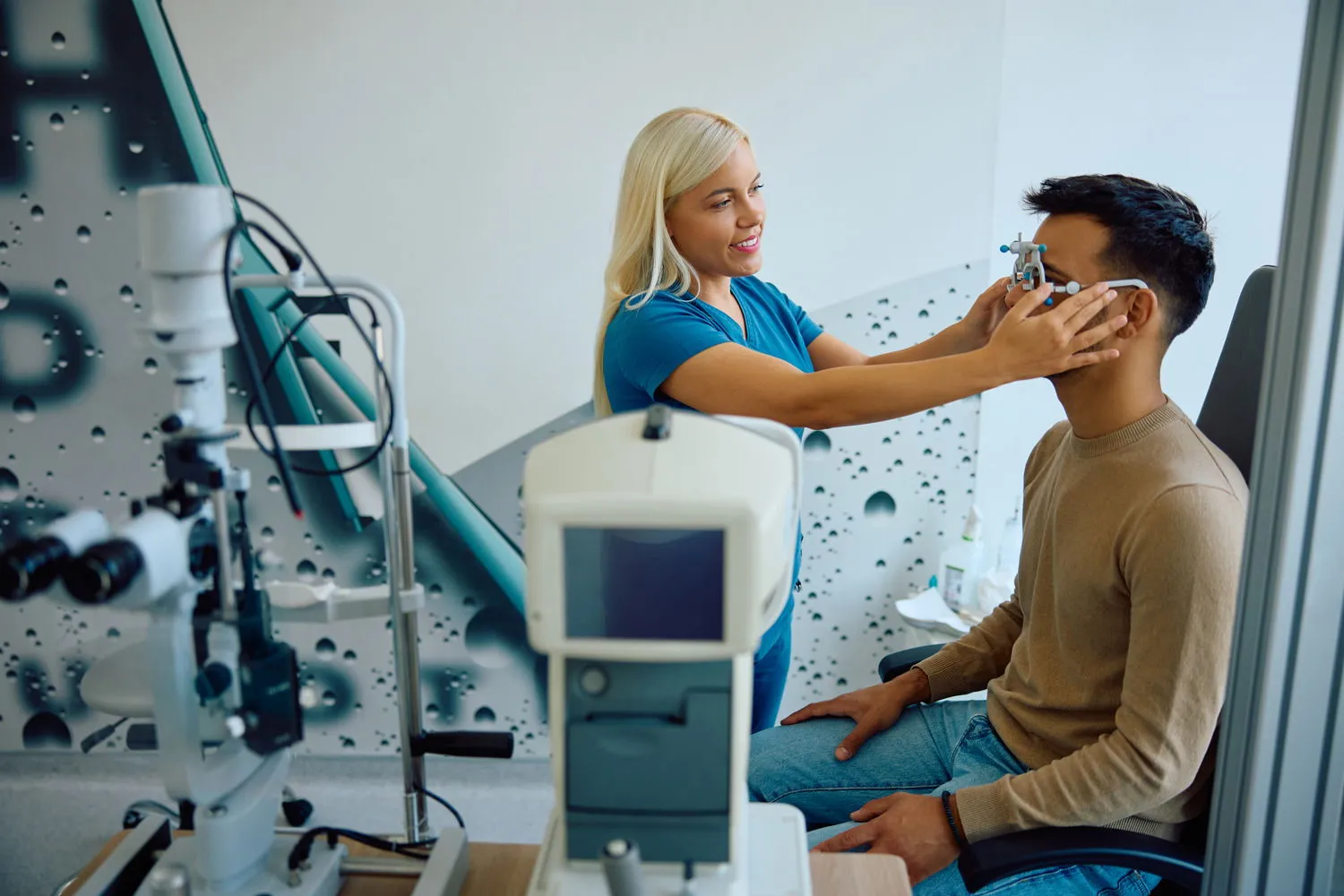
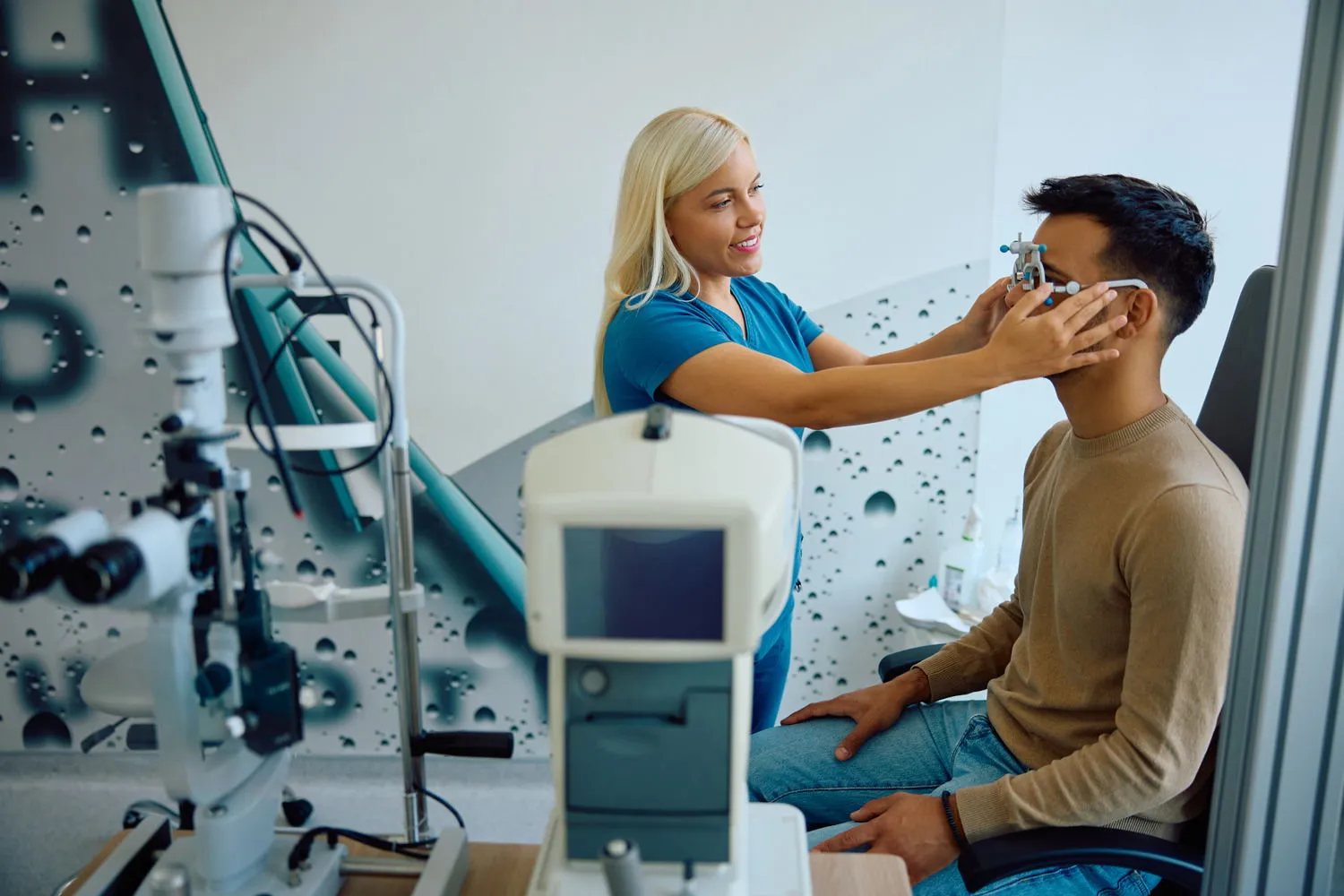
Virtual assistants play many roles in an ophthalmology clinic, often being the first point of contact in the patient experience. They handle various administrative tasks, from billing to scheduling appointments to patient intake, electronic health record keeping, and sometimes preliminary patient education or counseling. Each of these roles involves varying levels of exposure to sensitive patient information and carries specific compliance and security concerns.
When a VA schedules an appointment, for example, they need access to patient information like names, contact details, and in some cases, the reason for the visit. During patient intake or when maintaining patient records, they may have access to more detailed personal health information, which is more sensitive and subject to stricter regulations like being HIPAA compliant.
Some VAs have roles that require them to interact with patients in ways that impact their medical outcomes. For example, a VA might be tasked with explaining preparatory steps for an eye examination or advising patients on post-procedure care. Miscommunication or misunderstandings in such scenarios can lead to non-compliance with care protocols and even poor patient care.
Understanding these roles and associated data access levels is the first step in establishing robust compliance and security practices. This understanding can help identify potential points of vulnerability and tailor your training and security protocols to address them effectively. The training should address the specific data protection regulations relevant to their roles. Regular training updates should be implemented to ensure the VA is aware of any changes in regulations or clinic practices.
Next, you must ensure that your VAs’ actions align with your practice’s compliance requirements and patient data protection regulations.
How Do You Secure Communications and Data Management?
Communication and data management are two critical areas to focus on for anyone in the healthcare industry. These are the main channels through which information flows; hence, they require robust security measures.
This includes video conferencing, instant messaging, email, and any other forms of communication your clinic may use. Each channel should be encrypted and monitored for any signs of data breaches or unauthorized access. A policy should be in place for sharing sensitive information, ensuring it’s only done through secure means. For example, using personal email accounts or non-secure platforms should be strictly prohibited for official communication, especially if it contains personal information.
When dealing with VAs located overseas, it’s crucial to understand and manage the risks associated with cross-border data transfers. Countries have different data protection laws and regulations the protect personal data. Cross-border patient data transfer could expose it to different jurisdictions. To mitigate this, you should ensure that data transfers are secure, encrypted, and comply with all relevant regulations. Sometimes, you might need specialized secure data transfer tools or services.
To further enhance data security, utilize reliable tools and technology that ensure secure communication and data encryption. Conducting regular audits of VA activity helps detect any unusual actions or potential breaches. It’s also necessary to have a system in place for immediate action if a data breach occurs.
How Should You Manage Data Backups and Recovery?
If VAs are responsible for managing or accessing backed-up data, ensuring secure, encrypted access becomes crucial. Differences in time zones may affect backup schedules and immediate availability for recovery efforts.
The responsibilities for managing and executing backups should be clearly defined before hiring and may need to account for VAs’ work schedules across different time zones. Your recovery plan should be robust enough to ensure swift restoration of critical data irrespective of where your VAs are based. This includes data from your patient portal, billing systems, and similar critical systems. Training VAs on their role in this process and in initiating a recovery in case of data loss is a crucial element of compliance.
How Do You Navigate Cultural and Language Differences?
Cultural and language differences between your local team and overseas VAs can have direct and indirect implications for security and compliance. Misinterpretations due to language barriers can lead to mistakes in data entry, miscommunication of sensitive information, or even non-compliance with procedures, all posing potential security risks. Cultural differences in work habits and ethics may also impact adherence to data protection norms.
To ensure security and compliance, it’s necessary to have cultural and language training and communication strategies in place. VAs should receive comprehensive training on HIPAA compliance or other relevant regulatory standards, with language-appropriate materials and verification of understanding. Regular, clear communication and cultural sensitivity training can help mitigate miscommunications and foster an understanding of shared security responsibilities.
How Do You Ensure Continuity of Care with Virtual Assistants?
You may use VAs at your practice to handle administrative tasks, such as scheduling appointments or billing, or assist with patient outreach and education. However, clinical decisions must remain with a qualified medical professional. This delineation of work scope and limitations ensures the maintenance of quality patient care.
Procedures should be in place for transferring tasks from VAs to local staff when necessary. Situations like complex medical cases, patient-specific inquiries, or scenarios requiring a personal touch warrant a smooth transition to a local team member to complete the task.
Unforeseen circumstances like illness, internet outages, or other emergencies could render a VA unavailable. To ensure uninterrupted patient care, implement backup plans, such as training other staff members to perform the VA’s tasks or keeping backup VAs on call.
What Ethical and Contractual Considerations Apply?
Hiring virtual assistants, especially those overseas, brings a unique set of ethical and contractual considerations. Here are some key points to consider:
-
Overseas VAs often come from different cultural backgrounds and socio-economic conditions. Ensuring these individuals are given fair pay, reasonable working hours, and decent working conditions is important. This is an ethical imperative and helps maintain their motivation and productivity, which are key to them delivering on patient satisfaction.
-
Comprehensive contractual agreements with your VAs should include clauses about data privacy, breach notification procedures, and service level agreements (SLAs). It’s also beneficial to clearly outline the VA’s role and responsibilities, including what types of information they will handle and the processes they need to follow. Obtaining appropriate insurance may be necessary. Consulting with legal experts can be helpful to ensure all legal aspects are covered in your VA contracts, especially when dealing with VAs based in different jurisdictions.
-
If your VAs are based overseas, their work might be subject to different legal jurisdictions, which can complicate data privacy and compliance. You may need to consult legal experts to understand how to navigate these complexities.
-
An NDA can be a useful part of your contractual agreement with VAs. This legal document will require the VA to keep confidential any sensitive information they come across during their work.
Walking the walk of compliance and data security
What we shared scratches the surface, which is crazy, considering this article is long. There is much to know, stay up on, and keep balanced. For some eye care clinics, the best option is to partner with someone that can help.
Hiring a reputable and experienced vendor can provide eye care clinics with access to trained and skilled virtual assistants. They can also benefit from the vendor’s expertise in managing security and compliance, which is especially helpful for clinics needing more resources or expertise to manage these aspects.
When considering outsourcing VA services, a thorough evaluation of potential VA provider should include understanding their recruitment and training processes. Do they ensure their VAs have the necessary skills and knowledge to handle their responsibilities? What kind of ongoing training and support do they provide?
Investigate their data protection measures. How do they ensure secure communication with patients and data management? What measures do they have in place for backup and recovery for a client? Ask for information about their experience with a healthcare provider. Do they understand and comply with healthcare-specific regulations, such as HIPAA? Are they experienced in managing the specific challenges of healthcare settings?
Look for vendors who not only provide satisfactory answers to these questions but demonstrate a proactive approach towards data security and regulatory compliance. The right vendor will be a partner who contributes to the effectiveness and efficiency of your clinic.
As you progress with compliance and security for VAs, let us know if we can answer any of your questions about the process or help in any way.